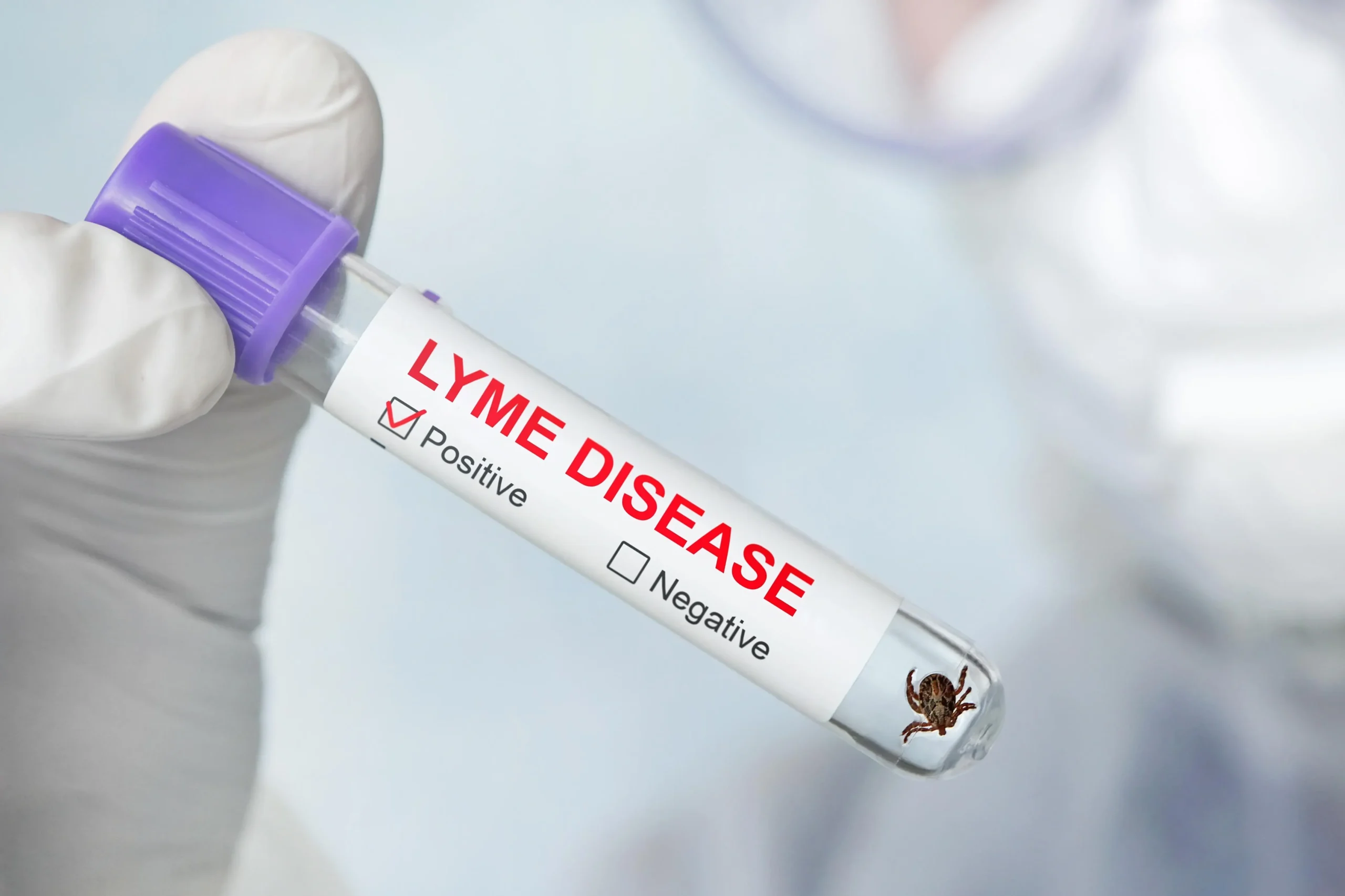



Full-spectrum testing goes beyond the traditional two-tier approach by using a more
comprehensive and integrative panel to detect Lyme disease and other tick-borne co-infections.
These tests aim to improve sensitivity and reduce false negatives. Some components of
full-spectrum testing include
At Infinity NAD Consulting, we provide expert Psychiatry, NAD+ Therapy, and Ketamine Therapy in Bellevue, WA, offering personalized, evidence-based care tailored to your unique needs and goals

DISCLAIMER: NAD+ qualifies as a supplement under FDA guidelines. These statements have not been evaluated by the Food and Drug Administration. Intravenous NAD+ therapy is not intended to diagnose, treat, cure or prevent disease.